Tickborne Illnesses

Current Activity
- 5/5/2025: Montanans have already begun reporting and submitting ticks for the 2025 season. Be prepared before engaging in outdoor activities by reviewing important information below.
Tickborne Surveillance Dashboard
About Ticks and Tickborne Illnesses
Found a tick? Share information about where and what kind of ticks you found here! Notifying us of what types of ticks you found allows us to better understand what kinds of diseases that are spread by ticks may be present in Montana.
Tips for Taking Photos of Ticks- Download Instructions Here!
- Photograph the tick against a solid white (or light colored) background.
- Position the tick in the photograph so that it is next to an object with a standardized size, like a ruler or a coin.
- Avoid taking pictures while the tick is still attached to a human or animal as many important identifying features can be hidden.
- Avoid taking pictures where there is a shadow, where the tick is out of focus, or where the camera is too far away and cannot identify features.
- When are ticks active in Montana?
- Ticks are most active from April through July, but Montanans are most likely to encounter ticks in May. However, tick activity in Montana is very dependent on the weather: activity may increase anytime the temperature is above freezing, especially following multiple days above 45°F. Ticks are also likely to slow down when summer weather becomes too hot and dry.
- When ticks are not active, they are typically found hiding among leaf litter or on a host animal. Working and recreating outside with activities such as gardening, landscaping, and hunting may increase your chances of encountering a tick during the winter.
- Where can ticks be found in Montana?
- What type of tick may vary, but they can be found at any elevation and in both dry and wet regions of the state.
- What tick species can be found in Montana?
- Rocky Mountain Wood Tick (Dermacentor andersoni)
- American Dog Tick (Dermacentor variabilis)
- Soft Ticks (Ornithodoros spp.)
- Brown Dog Ticks (Rhipicephalus sanguineus)
| Disease/causal organism | Incidence in Montana | Symptoms | Tick vectors |
|---|---|---|---|
| Rocky Mountain spotted fever/rickettsiosis (a bacterium, Rickettsia rickettsii) |
Rare, much more common in some areas along the Atlantic coast. About 8 cases per year, on average, are reported in Montana. | Initially, a general feeling of malaise and/or aches. A characteristic rash develops, starting on the wrists and ankles and later spreading to the rest of the body, including palms and the soles of feet. High fever is associated with infections. | Rocky Mountain wood tick, American dog tick. |
| Tularemia (a bacterium, Francisella tularensis ) |
Rare; only 5 cases on average are reported in Montana. Can be widespread in wild animals, particularly rabbits. | Sudden high fever, general weakness and swelling/pain of the lymph nodes. | Rocky Mountain wood tick, American dog tick. Most human infections occur from contact with the blood of infected animals (e.g., while skinning rabbits). |
| Colorado tick fever/biphasic fever (a virus) |
Rare; only 4 cases, on average, are reported in Montana. | Generally flu-like, including aching, fever, chills and fatigue. This typically lasts for 1 to 3 days. More severe complications sometimes develop. | Rocky Mountain wood tick, American dog tick. |
| Tick-borne relapsing fever/borreliosis (a bacterium, Borrelia hermsii) |
Very rare. | Rapidly developing fever 3 to 10 days after initial infection. Fever declines after about 4 days but may recur in multiple cycles. | Soft ticks of the genus Ornithodoros that are associated with rodents (e.g., chipmunks, pine squirrels). Human infections typically occur when camping in rustic cabins inhabited by infected rodents. |
| Lyme disease (a bacterium, Borrelia burgdorferi) | Most common tickborne illness in Montana residents even though all cases acquired disease out of state. Thirteen cases on average. Most US cases are from the northeastern, mid-Atlantic and north-central US. | Symptoms that occur 3 – 30 days after tick bite include fever, chills, headache, fatigue, muscle and joint aches. Rash occurs in 70% - 80% of infected cases. It is 12 inches or more and may be located on any area of the body. Later signs and symptoms severe headaches and neck stiffness, arthritis with joint swelling, and facial or Bell ’s palsy. | Blacklegged tick or deer tick. Not found in Montana. Most people infected by immature ticks that are less than 2mm in size. |
Updated 05/01/2024
What You Need to Know
- Wear an EPA registered insect repellent
- Treat clothing and gear with products containing 0.5% permethrin
- Check for ticks often
- Shower soon after being out doors
- Put clothing in the dryer for 10 minutes after being outdoors to kill ticks
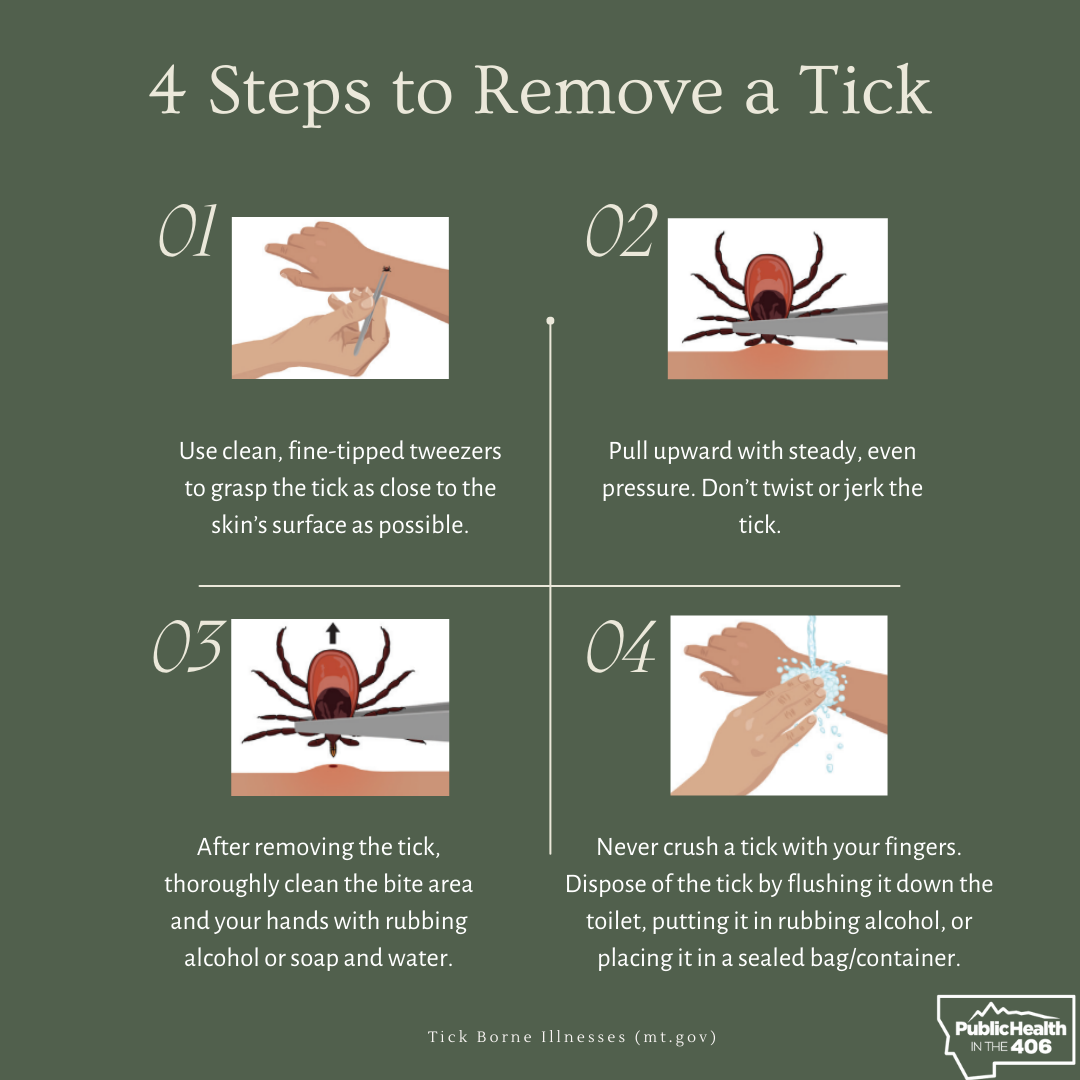
- Use clean, fine-tipped tweezers to grasp the tick as close to the skin’s surface as possible.
- Pull upward with steady, even pressure. Don’t twist or jerk the tick; this can cause the mouth-parts to break off and remain in the skin. If this happens, remove the mouth-parts with tweezers. If you cannot remove the mouth easily with tweezers, leave it alone and let the skin heal.
- After removing the tick, thoroughly clean the bite area and your hands with rubbing alcohol or soap and water.
- Never crush a tick with your fingers. Dispose of a live tick by
- Putting it in alcohol,
- Placing it in a sealed bag/container,
- Wrapping it tightly in tape, or
- Flushing it down the toilet.
The most common symptoms of tick-related illnesses include:
-
Fever/chills. All tickborne diseases can cause fever.
-
Aches and pains. Tickborne diseases can cause headache, fatigue, and muscle aches. People with Lyme disease may also have joint pain.
-
Rash. Lyme disease, Southern tick-associated rash illness (STARI), Rocky Mountain spotted fever (RMSF), ehrlichiosis, and tularemia can cause distinctive rashes.
Your healthcare provider should evaluate the following before deciding on a plan for treatment:
-
Your symptoms,
-
the geographic region where you were bitten, and
-
lab tests, depending on the symptoms and the geographic region where you were bitten.