Content Notice: This site contains HIV or STD prevention messages that may not be appropriate for all audiences. Since HIV and other STDs are spread primarily through sexual practices or by sharing needles, prevention messages and programs may address these topics. If you are not seeking such information or may be offended by such materials, please exit this website.
Concerned you might be infected with HIV? Find a testing site near you.
Visit the HIV Resource Library
If it has been less than 72 hours since you were exposed, there is medicine you can take to prevent infection. Click on the banner above for more information.
Are you an HIV prevention provider in need of HIV counseling, testing, and referral training (CTRS)? Head here for the self service eLearn module.
7 FACTS ABOUT HIV, the virus that causes AIDS
1. What is HIV? 
HIV stands for human immunodeficiency virus. It is the virus that can lead to acquired immunodeficiency syndrome or AIDS if not treated. Unlike some other viruses, the human body can’t get rid of HIV completely, even with treatment.
With treatment, HIV is a chronic condition, and most people who are HIV-positive, stay healthy for a long time with proper medical care.
2. Can it be cured?
No over the counter medication, prescription medication or alternative medicine will cure HIV or AIDS. Although a cure does not yet exist, taking HIV medicine as prescribed helps people living with HIV to live a long, healthy life and protect their sex partners from HIV.
 HIV can be controlled with proper medical care. The medicine used to treat HIV is called antiretroviral therapy or ART. According to the Centers for Disease Control (CDC), if people with HIV take ART as prescribed, their viral load (amount of HIV in their blood) can become undetectable. If it stays undetectable, they can live long, healthy lives and have effectively no risk of transmitting HIV to an HIV-negative partner through sex.
HIV can be controlled with proper medical care. The medicine used to treat HIV is called antiretroviral therapy or ART. According to the Centers for Disease Control (CDC), if people with HIV take ART as prescribed, their viral load (amount of HIV in their blood) can become undetectable. If it stays undetectable, they can live long, healthy lives and have effectively no risk of transmitting HIV to an HIV-negative partner through sex.
ART is recommended for all people with HIV, regardless of how long they’ve had the virus or how healthy they are.
If you are affected by HIV or know someone affected by HIV, please visit I'm HIV+, Now What? Go to GetTested.mt.gov to find case managers in Montana, get enrolled in a treatment program and learn more about HIV in Montana.
3. How is HIV spread?
If you have sex or share drug injection needles with people who could be infected with HIV, you are at a high risk of contracting HIV  yourself. Read more, on how HIV is spread.
yourself. Read more, on how HIV is spread.
When it comes to HIV, your overall sexual health is important. If you have another sexually transmitted disease (STD) like syphilis, gonorrhea or chlamydia, then you are more likely to become infected with HIV.
Fortunately, today there more tools than ever to prevent HIV. In addition to abstinence, limiting your number of sexual partners, never sharing needles, and using condoms the right way every time you have sex, you may be able to take advantage of newer pre-exposure prophylaxis (PrEP)medicines such as and post-exposure prophylaxis (PEP).

4. Test today. Don't delay.

Everyone should get tested at least once, and people at high risk should be tested at least once a year.
It is important for everyone to know their HIV status. Getting an HIV test is the first step for people living with HIV to get care and treatment and control the infection.
- The CDC says, All adults and adolescents from ages 13 to 64 should be tested at least once for HIV.
- Anyone who has unsafe sex or shares injection drug equipment should get tested for HIV at least once a year.
- Men who have sex with men should have an annual screening for HIV. Some gay and bisexual men may benefit from more frequent testing (for example, every 3 to 6 months).
- To find a testing site near you, go to GetTested.MT.gov
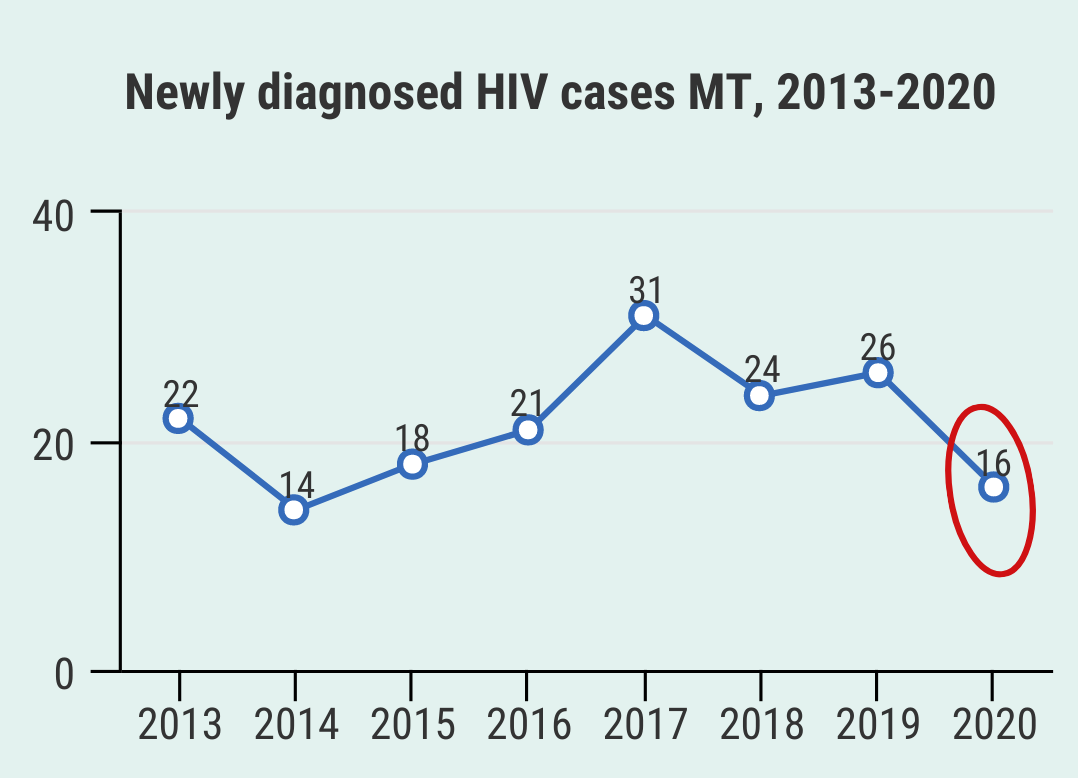
5. How common is HIV in Montana?
It is very likely the COVID pandemic decreased the number of 2020 HIV tests in Montana.
Of those newly infected, there were:
- 14 men and 2 women.
- 12 out of 16 were men who have sex with men (MSM) or MSM who also inject drugs.
15 were Non-Hispanic/white and 1 was Hispanic of any race.
The % of people who had developed AIDS at the time of diagnosis went from 23% to 37% in 2020.
These are small numbers and drawing conclusions should be done with caution.
6. How soon after exposure can I know if I have HIV?
If you may have been exposed in the last 72 hours, talk with your provider right away about post-exposure prophylaxis (PEP). Read more information about PEP in fact #7 or on our PEP page.
No HIV test can detect HIV immediately after infection. The time between when a person may have been exposed to HIV and when a test can tell for sure if they have it, is called the window period. The window period can be up to 90 days, varies from person to person, and depends on the type of test--some tests have a much shorter window period. Talk with your provider about when to return for another HIV test and read more about HIV testing.
7. How can I reduce my risk?
Today, more tools than ever are available to prevent HIV. You can choose not have sex, limit your number of sexual partners, never share needles, and use condoms the right way every time you have sex. You may also be able to take advantage of HIV prevention medicines.
- Pre-exposure prophylaxis (PrEP) is a daily medication taken by people at a very high risk for HIV. It greatly reduces the risk of HIV infection, if taken every day. Daily PrEP reduces the risk of getting HIV from sex by more than 90%. Among people who inject drugs, it reduces the risk by more than 70%. Your risk of getting HIV from sex can be even lower if you combine PrEP with condoms and other prevention methods. Any provider can prescribe PrEP. If you would rather work with someone besides your primary provider, find one near you, at GetTested.MT.gov under the PrEP tab.
- Post-exposure prophylaxis (PEP) is a medication taken as soon as possible, within 72 hours after being exposed to HIV. It is a once daily pill taken for 28 days and is effective in preventing HIV when taken correctly, but not 100%.
- Get tested and treated for syphilis, gonorrhea and chlamydia, because having an STD can increase your chances of getting HIV.
- There is currently no vaccine that will prevent HIV infection.
- If you are living with HIV, there are many things you can do to stay healthy and not infect others. Find out more at I'm HIV+, Now What?.
- Learn more about how to protect yourself and get information tailored to meet your needs from CDC’s HIV Risk Reduction Tool .
- Be in a monogamous relationship with an HIV negative partner.
- Use condoms the right way every time you have sex.
- Reduce your number of sexual partners.
- If you are HIV-negative and your partner is HIV-positive, encourage your partner to get and stay on treatment. If taken as prescribed, HIV medicine (ART) can lower the amount of HIV in the blood, (viral load), to where it cannot be detected. According to the CDC, “People with HIV who get and keep an undetectable viral load can stay healthy for many years and have effectively no risk of transmitting HIV to an HIV-negative partner through sex.”
Treatment only works only as long as the HIV-positive partner gets and keeps an undetectable viral load. Up to one-third of people in HIV care don’t keep an undetectable viral load.
If having an undetectable viral load status is your only prevention method, the HIV+ partner needs to take their medicine every day, visit provider regularly, and get a viral load test as recommended. “Blips” or small increases in viral load can increase the risk of infecting the HIV-negative partner. To avoid this possibility, people who are HIV-negative, can use additional prevention options such as condoms or PrEP.
Do you inject drugs?
- Find a Syringe Services Program at GetTested.MT.gov and click on the Syringe Services tab.
- Find more information about protecting yourself from HIV and Hepatitis C at HIV and Injection Drugs 101 fact sheet and
Hepatitis C & Injection Drug Use fact sheet - Click here for more ways to lower your risk of getting HIV.
- This HIV Risk Reduction Tool offers information tailored to meet your needs.
- Use these Substance Abuse Treatment locaters:
Behavioral Health Treatment Services Locator
SAMHSA's National Helpline – 1-800-662-HELP (4357) - Get more basic prevention information here .
Are you a man who has sex with men?
- Go to our PrEP page and learn how to access and pay for PrEP.
- Read this Gay and Bisexual Men's Health or PrEP 101 fact sheet
For more information
Have you been exposed to HIV or an STD?
Find a testing site near you
Cogswell Building
Room C-211
1400 Broadway
Helena, MT 59620
(406) 444-3565